DERMAN FILLER | May 17, 2021
What does Botox do
Entry made by
Empire Medical Training
The U.S. Food and Drug Administration first approved BOTOX® — commonly known by the generic name “Botox” — for clinical use in 1989 and has steadily expanded the range of clinical indications in the years since. At this point,
millions of people around the world have asked the question: “What does Botox do?”
The simple answer is, “quite a lot.” Botox is indicated for the treatment of a variety of neurological, musculoskeletal, and cosmetic
conditions. Many of the most common concern the skin, muscles, and nerves of the neck, face, and head: migraine, bruxism, TMJ, cervical dystonia, brow and forehead lines. Some, such as urinary incontinence, concern other areas
of the body.
Of course, like any medication that must be administered under the supervision of trained and licensed medical personnel, Botox is not to be taken lightly. Anyone considering Botox treatment for any condition deserves a more detailed explanation of what Botox does, how it works, how it’s administered, and the results — as well as the potential side effects — that patients
should expect.
What are the basics of Botox?
Botox is the generic name for a prescription medication derived from a neurotoxin produced by a particular strain of Clostridium botulinum bacteria.
Despite its origins, Botox has a low incidence of serious side effects when administered by trained medical professionals and aestheticians as indicated.
Botox
is indicated for the treatment of a variety of medical conditions. In a sense, these conditions offer a slightly longer answer to our question “What does Botox do?”
Because the absolute number of approved clinical
indications continues to grow and some indications are more common than others, this list of approved conditions is not comprehensive:
- Chronic migraine, defined as incidence greater than 15 days per month
- Spasticity
- Cervical dystonia (specifically to reduce neck pain and abnormal head positioning)
- Bladder dysfunction, including incontinence
- Axillary hyperhidrosis, or excessive sweating from the armpits
- Strabismus, or crossing/divergence of the eyes
- Blepharospasm, or involuntary closure of the eyelids
- Bruxism, or grinding of the teeth
- TMJ
- Certain facial lines and wrinkles, such as crows’ feet
- More detail about Botox’s indications for these conditions is available from RxList.
How does Botox work?
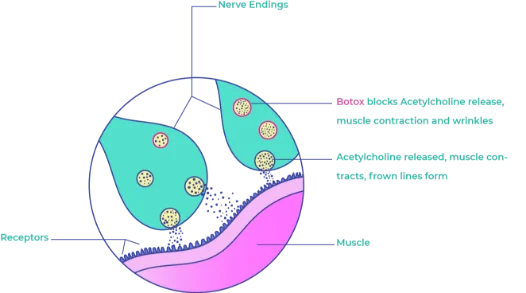
According to the American Association of Ophthalmology, Botox works by blocking nerve signals that would normally
cause muscles to contract. This temporarily weakens or paralyzes the affected muscles, producing the desired clinical effects.
Research published by the National Institutes of Health provides a more technical summary of what Botox does. Specifically, when administered to human muscle, the active ingredient in Botox (botulinum toxin) inhibits the release
of acetylcholine from presynaptic motor neurons at four different sites: the neuromuscular junction, autonomic ganglia, postganglionic parasympathetic nerve endings, and postganglionic sympathetic nerve endings responsible
for releasing acetylcholine.
In cosmetic applications, Botox’s visible or perceptible effects include the temporary lessening or disappearance of facial lines and wrinkles. In other clinical applications, they include
temporary reduction of pain and/or involuntary muscle activity and an associated reduction in symptoms of the condition(s) for which treatment is sought.
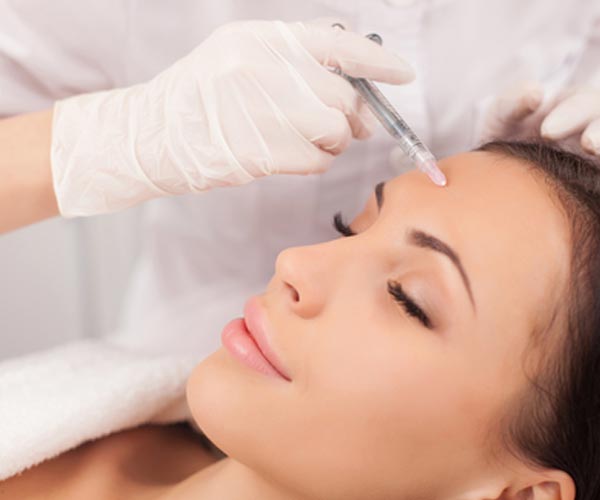
Botox treatment is administered by local subcutaneous injection to small muscle groups, most often on the
face, forehead, and neck. Each treatment’s effects usually last between three and twelve months, depending on dosage and condition, with four to six months a typical interval between treatments.
Botox’s clinical effects
typically take 24 to 72 hours to produce visible effects, according to findings published by the National Institutes of Health. Effects
typically peak within seven to fourteen days after treatment and remain noticeable for several months, albeit with gradual reversion to the pre-treatment baseline.
For the first 24 to 48 hours after treatment, Botox
patients should avoid exercise, strenuous activity in general, and further medical treatment or massage to treated areas of the body. This period of enforced rest reduces the risk of complications caused by the medication’s
spread to surrounding muscle groups (by reducing the risk of such spread).
Providers may also instruct their patients to take additional precautions after treatment. Common precautions include not touching the treated
area or areas nearby and remaining in a sitting or standing position (not laying down) for several hours following injection.
Can there be adverse reactions to Botox?
Botox can cause side effects even when administered as indicated under proper supervision. However, the overall incidence of such side effects is low. Most are mild and transient (temporary and resolving on their own). The incidence of more concerning side effects is rare

The most common mild to moderate side effects associated with Botox treatment include:
- Low fever
- Fatigue and other flu-like symptoms
- Headache
- Eye irritation, including excessive redness, dryness, or tearing
- Redness or bruising near the injection site (these reactions are usually associated with the use of blood thinning medications and alcohol)
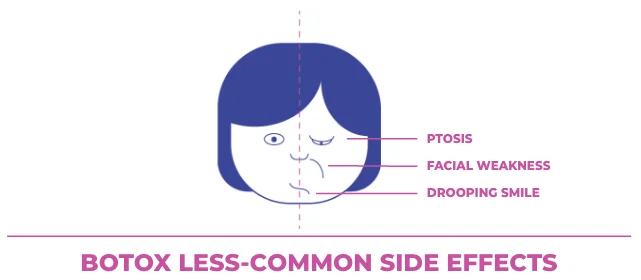
Certain less-common side effects are cause for concern and warrant consultation with a licensed medical professional:
- Ptosis, or drooping of the eyelids
- Facial weakness or numbness
- Drooping smile or drooling
- Weakness in the muscles of the arms, legs, or other areas not adjacent to the treatment site
- Changes in vision
- Difficult or painful breathing
- Difficulty speaking or swallowing
- Urinary incontinence (loss of bladder function)
Should anyone avoid Botox?
We now know what Botox does. The last questions we need to answer concern whether what Botox does makes the medication unsuitable for any prospective patients. When is Botox not indicated as a medical treatment, and should any prospective patients avoid
Botox entirely?
First, the limitations of Botox treatment — notably the fact that its effects are temporary and that it is correlated with a set of mostly mild side effects — do not mean
that the medication is not effective when administered as directed for treatment of the conditions for which it’s indicated.
That said, Botox’s indications do have some limitations. For example, Botox is not indicated
to treat all types of facial lines or wrinkles, nor is it approved for the treatment of any and all musculoskeletal conditions affecting the face, neck and head. (This is a common misconception.) All prospective Botox patients
should confirm with their medical provider or aesthetician that Botox is recommended for use in their specific situation.
Above all else, it is recommended that certain individuals and groups of individuals avoid Botox.
These include:
- People who are pregnant or may be pregnant
- People who are planning to become pregnant during the course of treatment
- People who are breastfeeding
- People with certain neurological conditions, including but not limited to multiple sclerosis, ptosis not caused by Botox treatment, facial paralysis or weakness not caused by Botox treatment, and myasthenia gravis