Platelet-Rich Plasma (PRP) therapy has emerged as a revolutionary treatment modality in pain management, offering patients a minimally invasive alternative to traditional interventions. As healthcare providers increasingly recognize the therapeutic potential of PRP, the demand for comprehensive training in this regenerative medicine technique continues to grow exponentially.
PRP therapy harnesses the body's natural healing mechanisms by concentrating platelets and growth factors from the patient's own blood. This concentrated solution is then strategically injected into damaged tissues, promoting cellular regeneration and reducing inflammation. For medical professionals seeking to expand their practice capabilities, understanding PRP applications in pain management represents a significant opportunity for both patient care enhancement and practice growth.
Understanding PRP Therapy Mechanisms
The science behind PRP therapy lies in the concentrated delivery of bioactive proteins and growth factors directly to injured tissues. When platelets are activated at the injection site, they release over 30 different growth factors that stimulate cellular proliferation, angiogenesis, and tissue repair.
The typical PRP preparation process involves drawing a small amount of the patient's blood, processing it through centrifugation to separate and concentrate platelets, and then injecting the resulting plasma into the target area. This autologous approach minimizes the risk of allergic reactions or disease transmission, making it an attractive option for many patients.
Research indicates that PRP can contain 3-5 times the normal concentration of platelets found in whole blood, significantly amplifying the body's natural healing response. This concentrated delivery system enables targeted treatment of specific pain sources while promoting long-term tissue health.
Clinical Indications for PRP in Pain Management
Musculoskeletal Conditions
PRP therapy has shown remarkable efficacy in treating various musculoskeletal conditions that cause chronic pain. Osteoarthritis, particularly in the knee joint, represents one of the most extensively studied applications. Clinical trials demonstrate significant pain reduction and functional improvement in patients receiving PRP injections compared to traditional treatments.
Tendinopathies, including tennis elbow, golfer's elbow, and Achilles tendonitis, respond exceptionally well to PRP therapy. The growth factors in PRP stimulate collagen production and promote tendon healing, often providing relief where other treatments have failed.
Other musculoskeletal applications include:
- Rotator cuff injuries and impingement syndrome
- Plantar fasciitis and heel pain
- Hip bursitis and greater trochanteric pain syndrome
- Chronic muscle strains and ligament sprains
- Joint capsule inflammation and synovitis
Spine-Related Pain Conditions
PRP injections have gained traction in treating spine-related pain conditions, particularly facet joint arthropathy and sacroiliac joint dysfunction. The anti-inflammatory properties of PRP can provide sustained relief for patients with chronic low back pain when combined with proper diagnostic evaluation.
Cervical spine conditions, including cervical facet joint pain and cervical disc degeneration, may also benefit from targeted PRP injections. However, these applications require specialized training and expertise in spinal anatomy and injection techniques.
Soft Tissue Injuries
Acute and chronic soft tissue injuries often heal inadequately due to poor blood supply or repetitive stress. PRP therapy can accelerate healing in these challenging cases by delivering concentrated growth factors directly to the injury site.
Common soft tissue applications include muscle tears, ligament injuries, and chronic wound healing. The regenerative properties of PRP make it particularly valuable for athletes and active individuals seeking faster recovery times.
Clinical Outcomes and Evidence Base
The evidence supporting PRP therapy in pain management continues to expand, with numerous systematic reviews and meta-analyses demonstrating its efficacy across various conditions. A recent comprehensive analysis of knee osteoarthritis studies showed that PRP injections provided superior pain relief and functional improvement compared to hyaluronic acid injections at 6 and 12-month follow-ups.
For tendinopathies, clinical studies report success rates ranging from 70-90% in achieving significant pain reduction and functional improvement. The duration of symptom relief typically ranges from 6-18 months, with many patients experiencing sustained benefits beyond initial treatment periods.
Key outcome measures consistently improved with PRP therapy include:
- Visual Analog Scale (VAS) pain scores
- Functional assessment scores (WOMAC, DASH, etc.)
- Return to activity timelines
- Patient satisfaction ratings
- Reduced need for pain medications
Long-term studies suggest that PRP therapy may slow disease progression in degenerative conditions like osteoarthritis, offering potential disease-modifying effects beyond symptomatic relief.
PRP Preparation Techniques and Protocols
Blood Collection and Processing
Successful PRP therapy begins with proper blood collection and processing techniques. Standard protocols typically involve drawing 30-60ml of peripheral blood into anticoagulant-containing tubes. The choice of anticoagulant and collection technique can significantly impact platelet recovery and activation potential.
Centrifugation parameters play a crucial role in achieving optimal platelet concentration. Most protocols employ a two-step centrifugation process: an initial soft spin to separate red blood cells, followed by a hard spin to concentrate platelets. Training programs must emphasize the importance of standardized processing protocols to ensure consistent therapeutic outcomes.
Activation Methods
Platelet activation can occur spontaneously upon injection or be induced through various activation agents. Common activation methods include calcium chloride, thrombin, or mechanical activation through needle passage. Each method has distinct advantages and considerations that practitioners must understand.
The timing of activation affects growth factor release kinetics and therapeutic duration. Some practitioners prefer immediate activation for acute injuries, while others utilize delayed activation protocols for chronic conditions requiring sustained growth factor release.
Injection Techniques and Anatomical Considerations
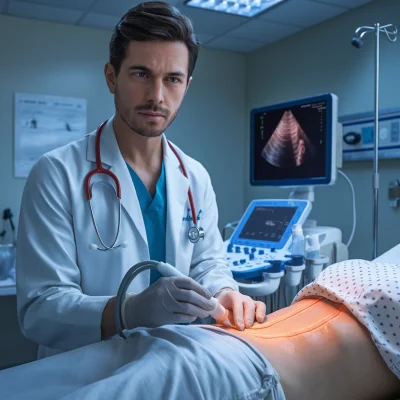
Precise injection technique is critical for optimal PRP therapy outcomes. Different anatomical locations require specific approaches and needle placements to ensure accurate delivery to target tissues. Ultrasound guidance has become the gold standard for many PRP injections, allowing real-time visualization of needle placement and tissue targeting.
Joint injections require thorough understanding of intra-articular anatomy and sterile technique. Practitioners must be familiar with anatomical landmarks, optimal needle entry points, and proper patient positioning for each injection site.
Soft tissue injections often utilize a fenestration technique, creating multiple small perforations in the target tissue to maximize growth factor distribution and stimulate healing response. This technique requires specialized training to avoid inadvertent injury to surrounding structures.
Training Requirements and Certification Pathways
Foundational Knowledge Requirements
Effective PRP training programs must establish strong foundational knowledge in several key areas. Practitioners need comprehensive understanding of platelet biology, growth factor mechanisms, and tissue healing processes. This scientific foundation enables informed clinical decision-making and appropriate patient selection.
Anatomy and injection skills represent another critical component of PRP training. Practitioners must demonstrate competency in musculoskeletal anatomy, sterile technique, and various injection approaches before advancing to clinical applications.
Hands-On Training Components
Comprehensive PRP training programs incorporate extensive hands-on components to ensure practical competency. These typically include:
- Blood collection and processing techniques
- Equipment operation and maintenance
- Injection skill development on anatomical models
- Ultrasound-guided injection training
- Patient assessment and selection protocols
- Complication recognition and management
[INTERNAL LINK: hands-on medical training importance]
Live patient demonstrations and supervised clinical experiences provide invaluable learning opportunities for developing confidence and competency in PRP therapy delivery.
Continuing Education and Advanced Training
The rapidly evolving field of regenerative medicine requires ongoing education to stay current with best practices and emerging techniques. Advanced training modules may cover specialized applications, combination therapies, and research developments in PRP therapy.
Many practitioners benefit from subspecialty training in specific anatomical regions or patient populations. Sports medicine applications, for example, require understanding of athletic injury patterns and return-to-play protocols.
Practice Implementation Strategies
Successful integration of PRP therapy into clinical practice requires careful planning and systematic implementation. Practitioners must consider equipment investments, staff training requirements, and workflow modifications to accommodate PRP procedures.
Patient education materials and informed consent processes need development to ensure proper expectations and understanding of treatment protocols. Clear documentation systems help track outcomes and refine treatment approaches over time.
Marketing and patient communication strategies should emphasize the evidence-based nature of PRP therapy while maintaining realistic expectations about treatment outcomes and timelines.
Future Directions and Advanced Applications
The field of PRP therapy continues to evolve with new preparation techniques, combination therapies, and novel applications emerging regularly. Advances in platelet concentration methods and growth factor analysis promise to optimize therapeutic outcomes further.
Combination approaches integrating PRP with other regenerative therapies, such as stem cell treatments or prolotherapy, show promise for enhanced healing responses in complex cases. These advanced techniques require specialized training and careful patient selection.
Research into personalized PRP protocols based on individual patient factors may revolutionize treatment approaches, requiring practitioners to stay current with evolving evidence and techniques.
Start Your PRP Training Journey Today
PRP therapy represents a significant advancement in pain management, offering patients effective, minimally invasive treatment options for various conditions. For medical professionals seeking to expand their practice capabilities and provide cutting-edge care, comprehensive PRP training is essential.
Empire Medical Training offers industry-leading PRP certification courses designed to provide the knowledge, skills, and confidence needed to successfully implement this transformative therapy. Our comprehensive curriculum combines scientific foundation, hands-on training, and ongoing support to ensure your success in PRP therapy delivery.
Contact Empire Medical Training today to learn more about our PRP certification programs and take the first step toward advancing your practice with this revolutionary pain management technique. Your patients deserve access to the latest regenerative medicine options, and we're here to help you provide them with exceptional care.